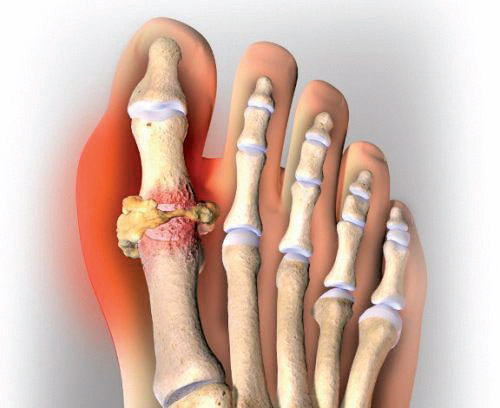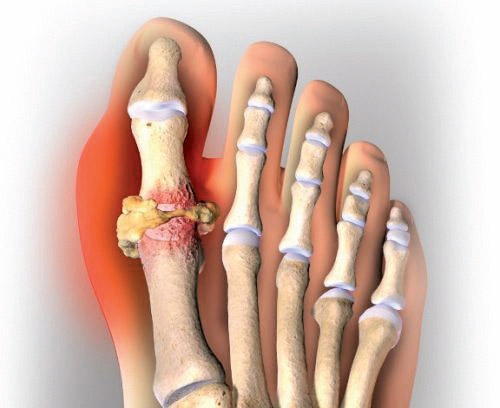
Gout, once relegated as a disease to the rich and prosperous, is now a condition that has dug its painful claws into the masses, affecting more than 3 million people every year. Gout is a form of arthritis, characterized by severe pain attacks, swelling, and tenderness in the joints. It often attacks the joint by the big toe, a condition known as podagra. Gout occurs when high levels of uric acid in the blood (which is a product of purine metabolism and is a normal component of urine) produces monosodium urate crystals to form and accumulate in and around the joints.
In normal circumstances, uric acid dissolves in the blood and passes through the kidneys, ending up in your urine. However, sometimes the body either produces too much uric acid or the kidneys cant/don’t excrete enough of it. There are certain factors that increase risk for gout:
- Diet (which I will delve more into)
- Obesity
- Medical conditions (i.e. uncontrolled diabetes mellitus, hypertension, metabolic syndrome, and chronic kidney disease)
- Certain medications (thiazide diuretics and low dose aspirin)
- Family history of gout
- Age and sex (gout tends to occur more often in men, as women tend to have lower uric acid levels. However, post menopause, women’s uric acid levels shoot up, rivaling men’s levels)
- Recent surgery or trauma
Referring back to the term, “disease of the rich”, gout attacks can be affected through purine intake, which can be found in some animal products, once thought to be only sectioned off to the wealthy due to their delicacy and isolating prices! Foods high in purines include organ and glandular meats (liver, kidney, and sweetbreads), red meats, anchovies, shellfish, sardines, tuna, alcohol (especially beer). Those kinds of foods can be expensive but these days are accessible to most. Medical professionals once advised against eating vegetables high in purines like mushrooms, spinach, and asparagus, but research has shown that they actually don’t increase risk of hyperuricemia. Other high-purine foods like oatmeal, nuts, and legumes don’t seem to increase risk as well.
Foods like coffee and cherries (especially tart cherry juice) have been researched on their efficacy on lowering gout risk. Hutton et al. (2018) states that increased coffee intake is associated with lower risk of gout and reduced serum urate concentrations. Coffee consumption seems to have an inverse association with gout risk (meaning, the more coffee you drink, the lower your risk becomes).
In regard to cherries, Zhang et al. (2012) conducted a case-crossover study (the case serves as their own control in the study) to examine the association between cherry intake and recurrent gout attacks. When cherry intake was combined with allopurinol use (one of the medication used to treat gout), the risk of gout attacks was 75% lower than during periods without either exposure.
There is some research stating that fructose intake (i.e. high fructose corn syrup, fruits, etc.) may increase uric acid levels, but more research needs to be done in order to confirm any recommendations.
If you do have gout, it’s important to reach out to your doctor to discuss your options. Medication/diet changes may be able to help exacerbate the pain associated with gout. Speak with a dietitian about making realistic diet changes if necessary when trying to relive gout-relayed symptoms.
Written by Melissa Papir Kolb, MS, RD