A case report and literature review: The American Journal of Orthopedics®
superior mesenteric artery syndrome as a complication of scoliosis surgery.
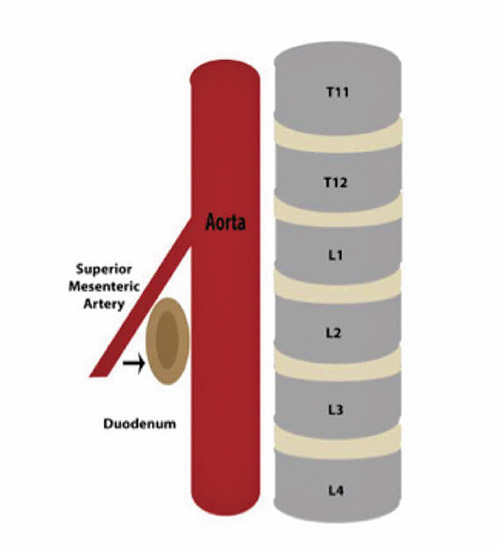
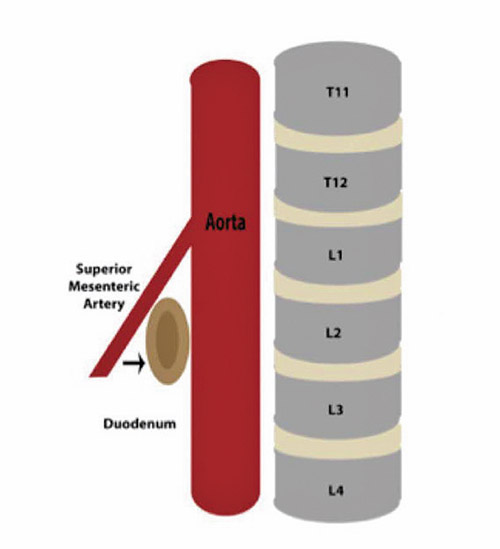
Superior mesenteric artery (SMA) syndrome is a rare and potentially life-threatening complication of scoliosis surgery. The anatomical relationship of the duodenum and the superior mesenteric artery, the correction of angular deformity of the spine, and the normal adolescent growth spurt all contribute to the condition.
Superior mesenteric artery (SMA) syndrome resulting from surgical treatment of scoliosis has been recognized in the medical literature since 1752. Throughout the literature, SMA syndrome variably has been referred to as cast syndrome, Wilkie syndrome, arteriomesenteric duodenal obstruction, and chronic duodenal ileus. We now recognize numerous etiologies of SMA syndrome, as several sources can externally compress the duodenum. Classic acute symptoms of bowel obstruction include bilious vomiting, nausea and epigastric pain. Chronic manifestations of SMA syndrome may include weight loss and decreased appetite. Our literature review revealed that adolescent growth spurt, height-to-weight ratio, and perioperative weight loss are risk factors associated with SMA syndrome after pediatric spine surgery.
Early recognition of the nonspecific symptoms of abdominal pain, abdominal distension, bilious or projectile vomiting, hypoactive bowel sounds, and anorexia plays a key role in post-scoliosis surgery and is crucial in preventing the severe morbidity and mortality associated with SMA syndrome.
Take-Home Points
- Adolescent growth spurt, height-to weight ratio, and perioperative weight loss are risk factors associated with SMA syndrome following pediatric spine surgery.
- Must recognize nonspecific symptoms such as abdominal pain, tenderness, distention, bilious or projectile vomiting, hypoactive bowel sounds and anorexia postoperatively.
- Complications of SMA syndrome can potentially lead to aspiration pneumonia, acute gastric rupture or cardiovascular collapse and death.
By Philip K. Louie, MD, Bryce A. Basques, MD, Adam Bitterman, DO, Shalin Shah, BS, Kishan Patel, BS, Isaac Abramchayev, PA-C, and Jonathan Lewin, MD